What are the Benefits of a Skin Cancer Self-Check?
The deeper a skin cancer, the longer it has been growing, the more difficult it is to treat, and the greater likelihood it has spread. By giving all parts of your body a regular check, you may be able to detect the early signs of skin cancer and increase the likelihood of successful treatment.
But there are also more subtle benefits to regular self-screening for skin cancer. By devoting the necessary time to the process, you stay aware of the dangers of skin cancer. As a result, you will be more likely to apply and re-apply sunscreens as appropriate, avoid the use of tanning beds, and take other steps to protect your skin from solar exposure. You benefit from preventing skin cancer before it can get started.
In terms of evidence, there is some evidence for the benefit of a skin cancer self-check & it is recommended in Australian guidelines.
There’s a degree of common sense involved in looking at the evidence for a self-examination of the skin. It would seem self-evident that regular self-examinations will pick up melanoma earlier than people who do not self examine their skin.
But let’s look at the evidence of benefit. An Italian study looked at 1240 people with newly diagnosed melanoma. All were taught to self-examine their skin after the diagnosis. Over the follow-up period, 47 had a recurrent melanoma. So here are the stats: The average thickness of the original melanoma was 1.31mm (that’s a significant melanoma), but the average thickness of the 2nd melanoma was 0.66mm – that’s an impressive reduction.
What are The Risks of a Skin Cancer Self-Examination?
Most skin cancers are not pigmented (dark), and it requires dermoscopy to diagnose an early BCC or SCC.
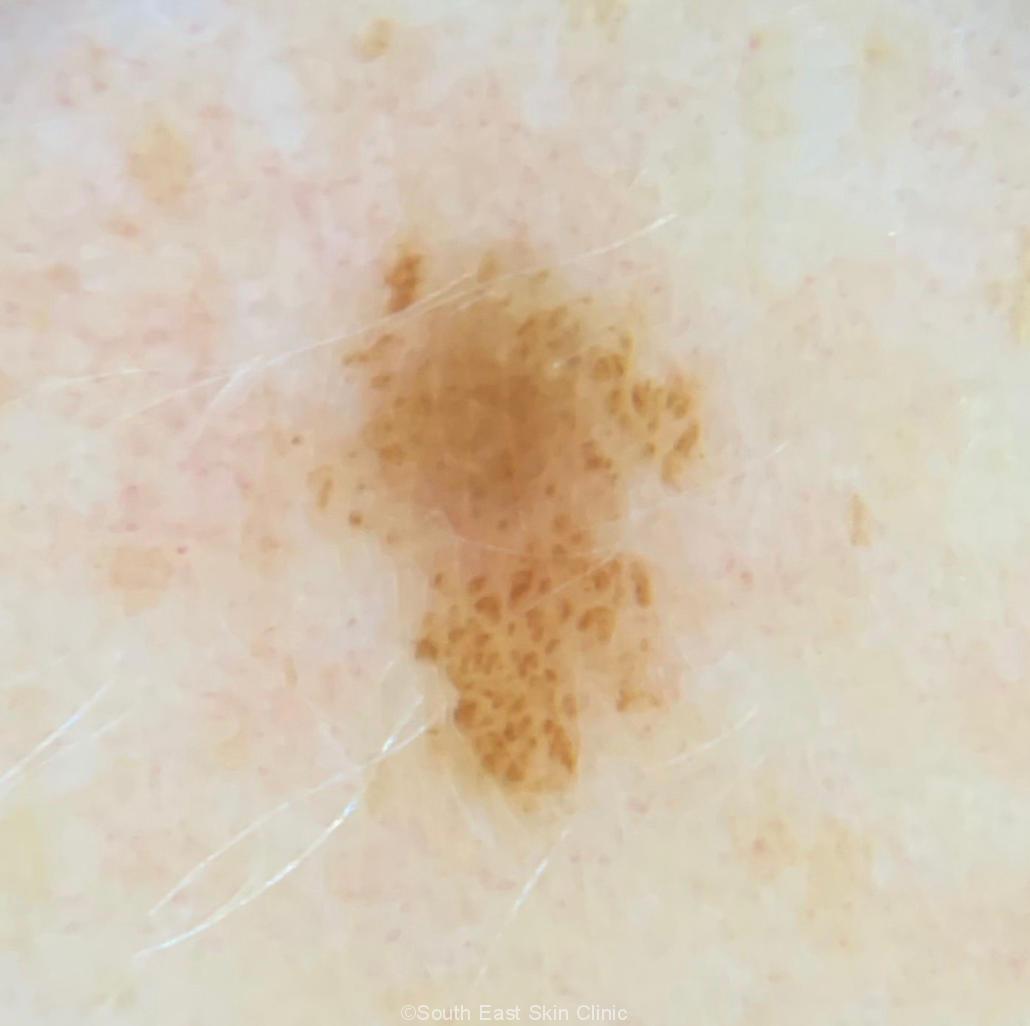
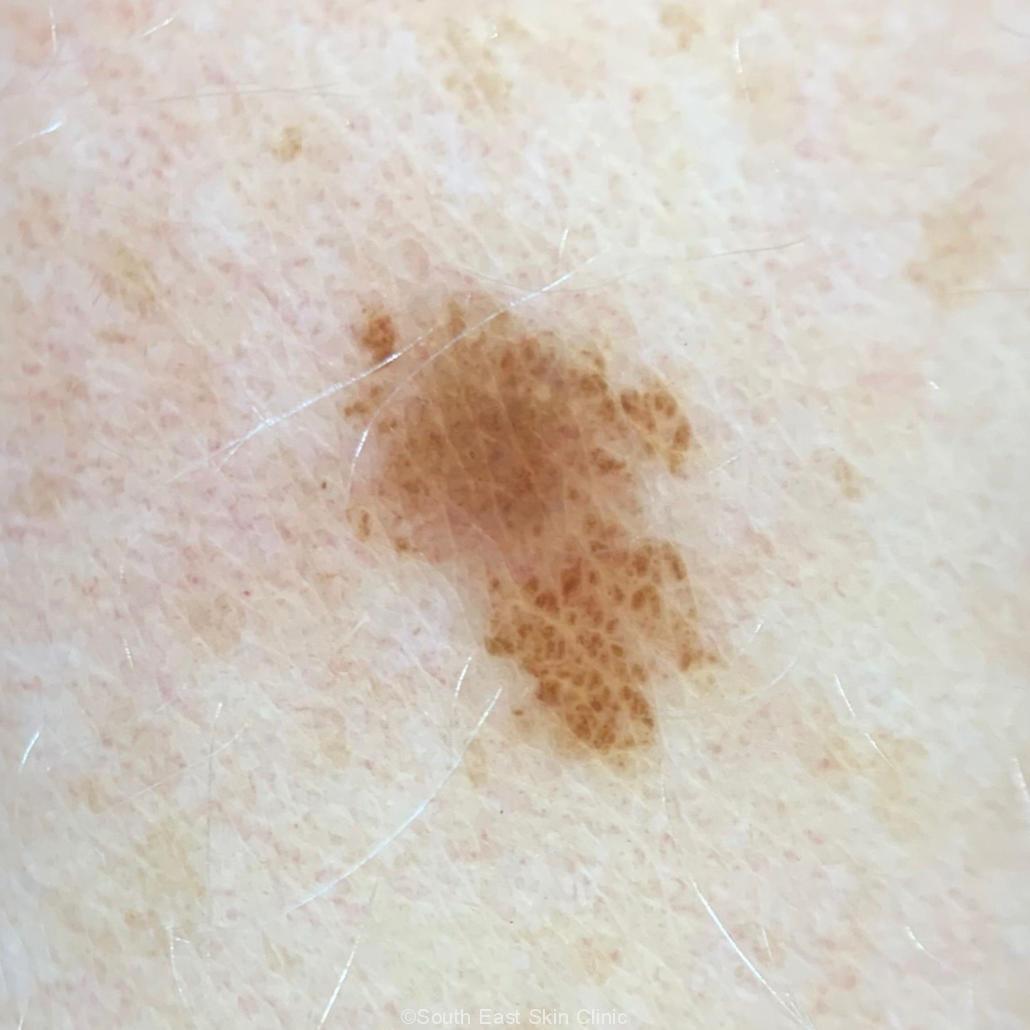
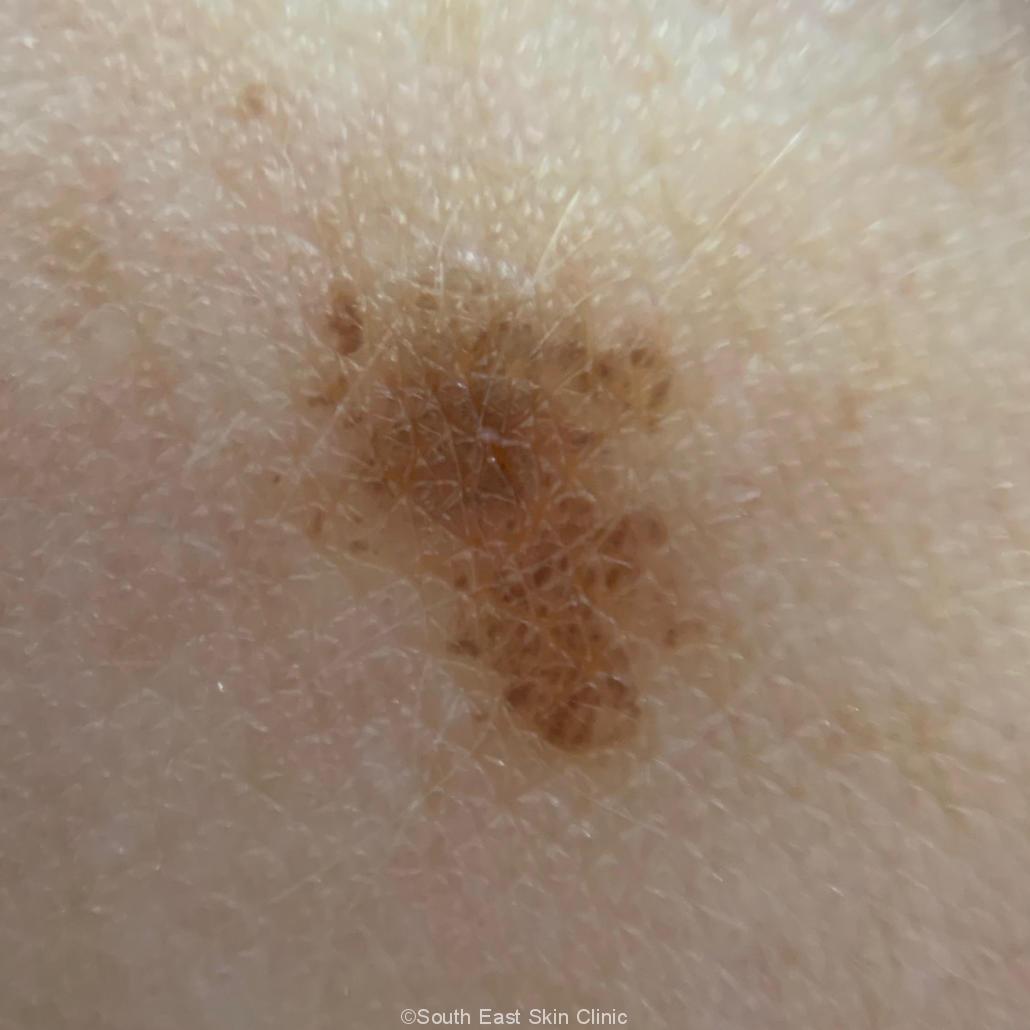
Early melanoma signs are subtle and require expert skin examination. Furthermore, uncommon types of melanoma, such as amelanotic and desmoplastic types, do not adhere to the usual ABCDE signs of melanoma and would probably be missed in a self-exam. Melanoma detected at a routine skin check is thinner compared with those detected by other means. Finally, most skin cancers are not melanoma, and SCC, in particular, kills more people than melanoma.
Let’s not forget non-melanoma skin cancer. In 2013 in Australia, there were 592 deaths from non-melanoma skin cancers (Cancer Council Australia). The signs of non-melanoma skin cancer are not straightforward though people who have a tendency to recurrent BCCs are often able to pick out another BCC. However, SCC is the more dangerous type of skin cancer & tends to grow rapidly – probably the first symptom will be an uncomfortable lump that has just appeared.
One of the risks of relying exclusively on self-checks for skin cancer screening is that you can’t identify it if you can’t see it. Our bodies have many bits that are difficult to see without a mirror. This includes not only your back but the back of your neck, the top of your head, behind your ears, etc. Cancers that arise in these areas may go undetected because you can’t easily see them when you inspect yourself.
Be mindful of the risk that self-checks can encourage people to take a wait-and-see approach that gives the cancer more time to spread.
Now let’s look at the evidence. A focused review of routine self skin-examination (SSE) in the diagnosis of melanoma was published in the international journal of dermatology in 2010. Of the studies examined between 1987 and 2007, the sensitivity of SEE for detecting melanoma ranged from 25% to 93%, whilst the specificity was 83% to 97%. This can be translated as follows: Take 100 people who have a melanoma but are unaware. The Self-check will pick up between 25% and 93% of these – let’s say around 50% to 60%.
So yes do your own skin checks on a regular basis, but this should not replace a regular skin examination.